GYN Surgery
Gynecologic minimally invasive surgery is the use of less invasive techniques to surgically treat gynecologic conditions. Minimally invasive techniques require no or only a few small incisions, rather than one large incision. Some of the procedures can be done on an outpatient basis, others may require a short hospital stay of one to two nights.
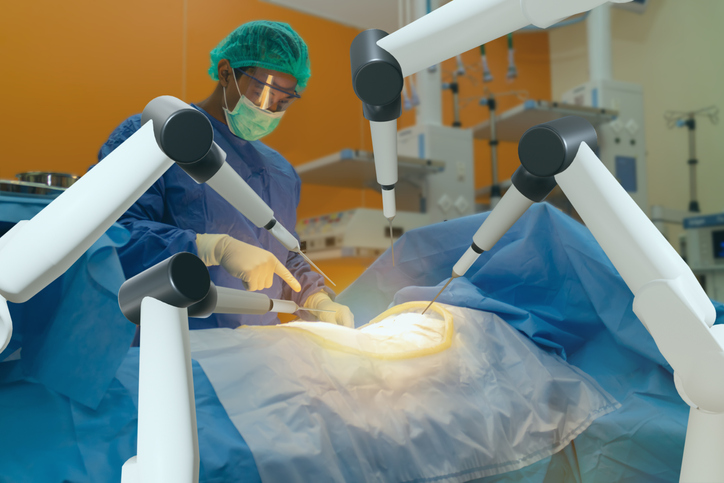
Delval OBGYN and Princeton Midwifery gynecologic surgeons are the Princeton area’s leaders in minimally invasive options to treat gynecologic conditions. Our physicians have specialized training and extensive expertise in techniques and technology such as the DaVinci robotic system for minimally invasive gynecologic procedures. Our surgeons are trained and able to treat complex gynecologic conditions, such as large fibroids and advanced endometriosis.
Gynecologic Minimally Invasive Surgery is a safer and more effective alternative to traditional open surgery. By avoiding a large stomach incision, you benefit from:
- Smaller incisions
- Less blood loss
- Less pain
- Shorter hospital stays
- Faster recovery and return to daily activities
- Reduced scar tissue
- Less risk of infection or other complications
Meet Our Surgical Team
Commonly Treated Conditions
We understand gynecologic surgery is very personal. Our care team is here for you during every step. We work closely with you to ensure that you always feel supported, empowered with information and comfortable with your choice. Our gynecologic surgeons will choose minimally invasive gynecologic surgery whenever possible.
The following are conditions our gynecologic surgeons can treat with minimally invasive surgery.
A condition where the fertilized egg attaches outside the uterus.
Tissue from the lining of the uterus, known as the endometrium, grows outside the uterus often causing chronic pelvic pain, and sometimes infertility.
Gynecologic Cancers, such as Cervical Cancer, Endometrial (Uterine) Cancer and Ovarian Cancer
Known as menorrhagia, irregular menstrual bleeding, and pain during periods, known as dysmenorrhea.
While most ovarian cysts are benign, it is important we check them to rule out cancer. It is especially important for postmenopausal women to be examined because they are at increased risk for ovarian cancer.
A bacterial infection of the female reproductive organs that is typically transmitted through sexual intercourse. Women with PID often experience no symptoms. A PID infection is often detected when women develop chronic pelvic pain or have trouble getting pregnant.
Happens when weakness in the vaginal wall allows organs such as the bladder, uterus or rectum to bulge into the vaginal canal. Childbirth, chronic cough, age and constipation can lead to this pelvic muscle weakness. This may occur more commonly within specific families or certain ethnicities.
Painful scar tissue can cause internal organs to be stuck together when they are not supposed to be. Most often, adhesions are the result of previous surgery, but some can occur following pelvic infection, and many times they accompany more severe stages of endometriosis.
Occurs in the lowest portion of the abdomen (below the belly button) and in the pelvis. Abdominal and pelvic pain can result from a wide range of conditions and disorders. The level of pain you experience does not always reflect the severity of the condition causing it. It is always important to seek medical care.
If you have gone into menopause, you should not experience menstrual bleeding. Not even spotting. Seek medical attention to determine the cause and treatment.
Noncancerous (benign) growths in or on the uterus. Fibroids almost never develop into uterine cancer, nor do they increase the risk of cancer, but they can affect your quality of life. Fibroids can range in size from microscopically small to large masses weighing several pounds that enlarge the uterus.
Develop when the lining of the uterus overgrows in a particular area. Uterine, or endometrial, polyps grow from the uterus wall and can be as small as a sesame seed or larger than a golf ball. Most uterine polyps are noncancerous (benign) but, occasionally, can be or become cancerous (malignant).
Uterine polyps have some symptoms in common with uterine fibroids, but the two types of growths differ in several ways: Polyps are growths of the uterine lining. Fibroids are growths of muscle tissue. Polyps are typically smaller than fibroids and often go away without treatment. Fibroids can shrink after menopause but do not go away. Polyps can lead to cancer and subfertility.
Types of Gynecologic Minimally Invasive Surgery
Our team is specially trained to diagnose and treat your gynecologic condition. Our surgeons work closely with you to evaluate your symptoms and other factors needed to determine what type of procedure is best for you. The type of procedure that best suits your needs depends on the type of condition, your overall health, symptoms and other factors.
DelVal OBGYN surgeons are highly accomplished and can offer the following types of Gynecologic Minimally Invasive Surgeries
A hysteroscope, a narrow, lighted camera, and instruments are inserted by the surgeon through the cervix to access the uterus without incisions.
Three to four incisions are made by the surgeon in the pelvic area to insert a laparoscope, a narrow tube with a lighted camera, and surgical instruments to access the surgical site.
The surgical site is accessed by the surgeon using both laparoscopy and the vaginal approach.
Your surgeon uses a robotic system with a console that provides magnified, high-resolution 3D imaging of the surgical site, and controls arms with miniaturized instruments to perform a laparoscopy.
A laparoscopy is performed with just one incision into the belly button (navel)
Vaginal Technique - a small incision in the vagina by the surgeon to access the surgical site.
Resources
Want to learn more? Follow the links below for more information about women’s gynecologic health, conditions, diagnosis and treatment options.