Author Archives: vlm
What to Expect at 37 Weeks Pregnant – Third Trimester Information

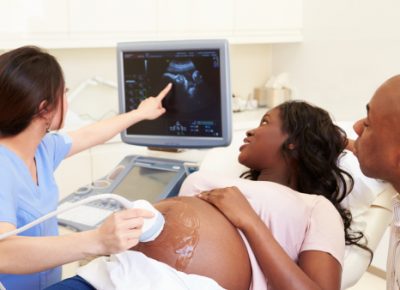
You are 37 weeks pregnant and your pregnancy is quickly coming to an end, but your little one still has a bit more growing to do. This week, your baby is probably gaining about a half an ounce each day, adding fat and plumping up before birth. Keep in mind that, although you are super close to your due date, your baby is still considered to be in the “early term” stage at this point. Your baby won’t be considered “full term” until week 39.
What are symptoms like at 37 weeks pregnant?
Pelvic pain or pressure. Is your baby sitting lower in your pelvis these days? This dropping — also called lightening or engagement — can occur a few weeks before your baby is born, and you might notice it if you feel a little extra pressure on your lower abdomen. This pelvic pain can even make it hard for you to walk. If pelvic pressure is causing you discomfort, a warm bath may provide some relief. Contact your healthcare provider for more advice on what to do to relieve pelvic or lower back pain.
Shortness of breath. Your baby might not have dropped yet and is pressing up against your lungs, making breathing a little more difficult. Try to rest more, move slowly and sit or stand up straight to help give your lungs more room to expand with each breath. Once your baby “drops” lower into your pelvis, this may take some pressure off your lungs and diaphragm, making it easier for you to breathe.
Nausea. Some moms-to-be experience nausea around 37 weeks pregnant, and it could be a sign that labor is about to start. Try to eat four or five smaller meals instead of three larger meals. Bland foods like rice, toast or bananas can also help get you through these bouts of nausea.
Snoring. This one might not trouble you as much as your partner. Most moms-to-be go through some breathing changes during pregnancy thanks to hormonal changes, and toward the end, some snoring is not uncommon as the mucus membranes in your nasal passages tend to dry out. Make sure you stay hydrated and use a humidifier in your bedroom.
Unstable on your feet. By now, your pregnancy weight gain means your center of gravity has shifted, making it easier for you to lose your balance. This extra weight from your baby, the placenta, amniotic fluid, and more can make it challenging to move around. Once your baby drops lower into your pelvis, the distribution of your weight may even change again, so be extra careful whenever you’re on your feet! To keep yourself steady, stand with your feet pointed in the same direction with your weight balanced evenly on both feet. Try not to tilt your pelvis forward or backward, and avoid lifting or carrying heavy or bulky items.
Contractions. At 37 weeks pregnant, you could start to feel contractions that you might recognize as being similar to menstrual cramping. Contractions that are irregular and go away when you move or change positions are likely Braxton Hicks “practice” contractions. But, if you feel contractions that occur regularly, get progressively stronger, and don’t subside if you move or change positions, you’ll want to call your healthcare provider for advice.
Practical plans for the birth
Still haven’t packed your hospital bag? Get to it! Your baby could arrive any day now.
This is also a good time to consider your support after the birth too. Who could you ask to help out every now and then?
Research your options for feeding your baby. The choice of breastfeeding or formula feeding is yours to make, but you may want to find out more about each. You can talk to your healthcare provider or a lactation consultant to get more information.
If you haven’t already purchased one, you’ll need a rear-facing car seat properly installed in time for your baby’s trip home from the hospital. Make sure the car seat you buy meets all safety standards.
You may want to ask for help from trusted friends, neighbors, or family members with things like grocery shopping, laundry, or looking after your older children or family pets in the first few weeks with your newborn. Make a list of what you might need help with so that your helpers know exactly what they can do to lighten the load.
Have additional questions about the third trimester? Planning a pregnancy? Would you like to meet with Providers and Other Parents?
Join us at Delaware Valley OB-GYN’s next Birth Babies and More Event on Tuesday, Dec. 5 at 6 p.m.
We’ll discuss the third trimester, labor, delivery and the exciting newborn period.
RSVP HERE
October Breast Cancer Awareness: Now is the Time to Schedule Your Annual Exam!

While breast cancer awareness articles and events are everywhere. What does breast cancer mean for you as an individual? It’s a scary thought and all too many women assume that it won’t happen to them. Fact is though, every two minutes a woman is diagnosed with breast cancer in the US. And – it is the most common cancer for women worldwide.
So, if you haven’t already, educate yourself in breast cancer awareness and find out your risk level. Get a medical check-up. And, if you need one, a mammogram. It might save your life.
Here are some Breast Cancer Awareness facts:
- Female breast cancer represents 15.2% of all new cancer cases in the U.S.
- 1 in 8 American women will develop breast cancer in her lifetime.
- Although far rarer (the risk is only 1 in 1000), an estimated 2,670 men will be diagnosed with this cancer this year.
- The disease takes the lives of more than 40,000 American women each year and has directly or indirectly touched almost all our lives.
- Education, fundraising and research has not resulted in a cure.
Breast Cancer Awareness: Early Signs
Early signs of breast cancer can be a lump in a breast, a painful breast or armpit or a discharge from the nipple. Even if none of these symptoms present themselves, a doctor should be visited to be sure. A doctor will most likely perform a manual exam and send you for a mammogram. A mammogram examination is painless and only takes about 10-20 minutes.
If any of these symptoms do present themselves there’s no need to panic. The pain can be a sign of a cyst or the lump can be benign. It’s always better to be sure by having a medical expert examine you.
Risk Factors for Breast Cancer
All women are at risk for breast cancer. Increased risk factors include a family history of cancer, atypical hyperplasia, delaying pregnancy until after age 30, no children or no breast-feeding, early menstruation (before age 12) late menopause (after age 55), current use (in the last 10 years) of oral contraceptives, more than 4 years of hormone replacement use, postmenopausal obesity, alcohol consumption, exposure to second-hand cigarette smoke, low physical activity and exposure to radiation.
These and other risk factors can have varying effects on the likelihood of developing breast cancer. It is important to remember that all risk factors are based on probabilities, and even someone without any risk factors can still get breast cancer. Proper screening and early detection remain the best weapons against mortality associated with this disease.
Scheduling an Annual Exam and Mammogram
The risk increases with age. That is why it is very important for all menopausal women to get regular mammograms.
A mammogram is a screening test which uses special X-ray images to detect abnormal growths or changes in breast tissue.
Mammography is your best defense because it can detect the disease in its early stages, before it can be felt during a breast exam. Research has shown that mammography can increase survival rates.
The American Cancer Society recommends women ages 40 to 44 should have a choice to start yearly screening mammograms if they would like. Women ages 45 to 54 should have a mammogram each year and those 55 years and over should continue getting mammograms every 1 to 2 years. You might need to start earlier if you have a family history and / or certain risk factors.
If you’ve never had a mammogram or you’re overdue, schedule an appointment with one of our women’s health experts for an evaluation.
Health Disclaimer. If you or any other person has a medical concern, you should consult with your health care provider or seek other professional medical treatment. Never disregard professional medical advice or delay in seeking it because of something that have read on this blog or in any linked materials.
Your Teen’s First Gynecologic Visit

Have you considered that Summer may be the best time for your teen’s first gynecologic visit? The dog days of summer are upon us. Are you enjoying lazy days at the pool, planned family vacations or busy times with kids active in sports and other camps? Why does it seem these days fly by and before you know it, the store aisles are filled with back-to-school supplies and fall clothes?
While this is a fun-filled time for your family – this is also the perfect time to consider your teenage daughter’s first gynecologic visit with us. Our expert physicians and midwives not only have the experience necessary to care for your teen but also are sensitive to her teenage gynecologic health needs.
We’ve provided answers to frequently asked questions below. However, we’re more than happy to schedule a first-time consult with your teen to answer her questions and put her at ease. Schedule your daughter’s first GYN appointment with us HERE. We’ll get her started on a healthy and empowered pattern of female wellness.
First Gynecologic Visit for Teens FAQs
Here are helpful answers to frequently asked questions originally posted on the American College of Obstetrician’s Website.
When should I have my first gynecologic visit?
An obstetrician–gynecologist (OB-GYN) is board certified in obstetrics and gynecology and certified nurse midwives (CNM”s) are registered nurses with graduate education in midwifery. OB-GYN’s and CNM’s specialize in the care of women’s health needs. Girls should have their first gynecologic visit between the ages of 13 years and 15 years.
Is it normal to be nervous before the first visit?
It is normal to feel nervous about your first visit. It may help if you talk about it with your parents or someone else you trust. You may want to let your doctor / midwife know you are nervous. He or she can help put you at ease.
What should I expect at the first gynecologic visit?
The first visit may be just a talk between you and your doctor / midwife. You can find out what to expect at future visits and get information about how to stay healthy. You also may have certain exams.
Your doctor / midwife may ask a lot of questions about you and your family. Some of them may seem personal, such as questions about your menstrual period or sexual activities (including vaginal, oral, or anal sex). If you are concerned about confidentiality, you and your doctor should talk about it before you answer any questions. Much of the information you share can be kept confidential.
What exams are performed?
You may have certain exams at the first visit. If you choose, a nurse or family member may join you for any part of the exam. Most often, these exams are performed:
- General physical exam
- External genital exam
You usually do not need to have a pelvic exam at the first visit unless you are having problems, such as abnormal bleeding or pain. If you are sexually active, you may have tests for certain sexually transmitted infections (STIs). Most of the tests that teens need can be done by the doctor with a urine sample. You also may have certain vaccinations.
What happens during a general physical exam?
During the general exam, your height, weight, and blood pressure will be checked. You also will be examined for any health problems you may have.
What are the pelvic exam and Pap test?
Even though you probably will not have a pelvic exam, you should know what one is. Another test that you will have later (at age 21 years) is a Pap test. This test checks for abnormal changes in the cervix that could lead to cancer.
What are vaccinations?
Vaccinations or immunizations protect against certain diseases. The following vaccines are given to all young women aged 11–18 years on a routine basis:
- Tetanus–diphtheria–pertussis (Tdap) booster
- Human papillomavirus vaccine
- Meningococcal vaccine
- Influenza vaccine (yearly)
- In addition to routine vaccines, special vaccines may be given to young women who are at an increased risk for certain diseases. Listed are some of these vaccines:
- Hepatitis A virus vaccine
- Pneumococcal vaccine
What special concerns can be discussed with my Ob-Gyn / Midwife?
Many young women share the same health concerns. Most of these concerns are a normal part of growing up:
- Cramps and problems with menstrual periods
- Acne
- Weight
- Sex and sexuality
- Birth control
- STIs
- Alcohol, drugs and smoking
- Emotional ups and downs
What can I do to stay healthy?
- Making good lifestyle choices can help you to be strong and healthy for years to come
- Maintain a healthy weight by eating a well-balanced diet and exercising often
- Avoid smoking, drinking alcohol, and using illegal drugs
- Seek help if you have emotional ups and downs or feel depressed
- Use birth control if you are having sex and do not want to have a baby
- Protect yourself from STIs by using a latex condom. Know your partners and limit their number
- Keep up with routine exams, tests, and immunizations
Here are some helpful terms:
- Birth Control: Devices or medications used to prevent pregnancy
- Cervix: The lower, narrow end of the uterus at the top of the vagina
- Condom: A thin cover for the penis used during sex to prevent sexually transmitted infections (STIs) and pregnancy
- Menstrual Period: The monthly shedding of blood and tissue from the uterus
- Midwife (CNM): A nurse with special training and education in women’s health
- Obstetrician–Gynecologist (Ob-Gyn): A doctor with special training and education in women’s health
- Pap Test: A test in which cells are taken from the cervix (or vagina) to look for signs of cancer
- Pelvic Exam: A physical examination of a woman’s pelvic organs
- Sexually Transmitted Infections (STIs): Infections that are spread by sexual contact
- Speculum: An instrument used to hold open the walls of the vagina
- Vagina: A tube-like structure surrounded by muscles. The vagina leads from the uterus to the outside of the body
- Vulva: The external female genital area
We’re more than happy to answer your questions. Contact us today. Call 609-896-0777 or schedule a consult HERE.
Don’t Suffer From Excessive Menstrual Bleeding (Menorrhagia)

If your periods are so heavy and or prolonged that they disrupt your normal daily activities, you may have excessive menstrual bleeding also known as menorrhagia. Symptoms of menorrhagia may also include cramping, pelvic pain and, in severe cases, anemia.
Excessive menstrual bleeding is a common condition that occurs for many of reasons. Two of the most common causes are a hormonal imbalance and uterine growths.
Hormonal Imbalances
Your menstrual cycle is controlled by hormones, including estrogen and progesterone. When these hormones are out of balance, they can cause heavy periods or bleeding between periods. Causes of hormonal imbalances may include:
- Hormonal changes in teens and in women nearing menopause
- Diabetes
- Thyroid disease
- Obesity
- Stress
- Strenuous exercise
- Anorexia (eating disorder)
Types of Uterine Growths
- Fibroids – benign (non-cancerous) growths in or near the uterus
- Polyps – growths that attach to the inner wall of the uterus and protrude into the uterine cavity
Treatment Options
There are medication and non-invasive treatment options available. Treatment options could include NSAIDs, oral contraceptives, oral hormones or a hormonal IUD.
You may need surgical treatment for menorrhagia if medical therapy is unsuccessful. Treatment options include:
Dilation and Curettage (D&C)
During this procedure, your doctor opens (dilates) your cervix and then scrapes or suctions tissue from the lining of your uterus to reduce excessive menstrual bleeding.
Uterine Artery Embolization
For women whose menorrhagia is caused by fibroids, the goal of this procedure is to shrink any fibroids in the uterus by blocking the uterine arteries and cutting off their blood supply.
Myomectomy
This procedure involves surgical removal of uterine fibroids.
Endometrial Ablation
This procedure involves destroying (ablating) the lining of your uterus (endometrium). The procedure uses a laser, radiofrequency or heat applied to the endometrium to destroy the tissue.
Endometrial Resection
We use the Myosure procedure to remove the growth on your uterus while preserving form and function of the uterus. Both endometrial ablation and endometrial resection benefit women who have very heavy menstrual bleeding.
Hysterectomy
This surgery to remove your uterus and cervix is a permanent procedure that causes sterility and ends menstrual periods. Hysterectomy is performed under anesthesia and requires hospitalization. Additional removal of the ovaries (bilateral oophorectomy) may cause premature menopause.
Many of these surgical procedures are done on an outpatient basis. Although you may need a general anesthetic, it’s likely that you can go home later on the same day. An abdominal myomectomy or a hysterectomy usually requires a hospital stay.
For those who require a surgical procedure, traditional open GYN surgery uses larger incisions for access to the uterus and surrounding anatomy which, ultimately, results in more pain, trauma and a longer recovery process.
Minimally Invasive Robotic-Assisted GYN Surgery
Drs. Pierce, Ung and Gamburg are the Princeton area’s most experienced GYN surgeons using the da Vinci® XiTM Surgical System for minimally invasive gynecologic surgeries.
Minimally invasive procedures like robotic-assisted GYN surgery are especially promising for women who would like to have children in the future. For instance, when removing fibroids – regardless of the size and location of the fibroid – the surgeon is able to better see where they are operating and to make precise movements to remove it, preserving the delicate structures of the pelvis and decreasing the chance of future complications.
The overall benefits of robotic-assisted GYN surgery include:
- Fewer complications
- Less blood loss and risk of infection
- Significantly less pain and scarring
- Shorter recovery time for a quicker return to normal activities
- A less invasive surgical option to get you back to your daily life
By operating with the da Vinci® XiTM Surgical System, our patients who suffer from excessive menstrual bleeding see noticeable benefits because incisions are smaller, pain is minimized and recovery time is reduced.
While clinical studies support the effectiveness of the da Vinci Xi Surgical System when used in minimally invasive surgery, individual results may vary. Surgery with the da Vinci Xi Surgical System may not be appropriate for every individual. Always ask your doctor about all treatment options, as well as their risks and benefits.
You don’t have to suffer from excessive menstrual bleeding any longer. To learn more about your treatment options, Contact Us for an Appointment HERE.
Is Choosing a Midwife Right for You?

We are one of the Princeton area’s leaders in establishing a model of care using both the skills of both the midwife and those of physicians in a collaborative manner to produce the best outcomes for our patients and their families. Our midwives are highly educated and trained medical professionals who have studied and graduated from some of the most respected formal education programs in the country. They are able to be designated as Nurse Midwives only because they have successfully completed a rigorous national certification examination.
A Midwife Offers an Elevated Model of Care
Our midwives are specialists in women’s health. Alongside our physician experts and support team, they provide primary and reproductive care to women of all ages. Midwives have particular expertise in normal pregnancy, labor, and delivery. Scientific studies have shown that care under a midwife significantly decreases the risk of medical interventions, including cesarean delivery. Our midwives do an extraordinary job caring for the patients in our practice.
Midwives and Childbirth
At Delaware Valley OB/GYN, we recognize that childbirth is a natural phenomenon and that most pregnancies are healthy ones. There are some pregnancies that do need extra medical attention and care. Our midwives work collaboratively with our physicians to recognize when a patient needs that extra attention. When our physician must assume a lead role due to the degree of increased pregnancy risk status, our midwives continue to participate in physical care, counseling, guidance, teaching, and support of our patients. It is always our intention, for our midwives and physicians to apply their expertise and to work jointly when caring for women with special medical needs.
Midwives and Gynecology
Additionally, our Nurse Midwives are a great option as providers for gynecologic care. Here are five reasons to consider a Nurse Midwife for gynecologic care:
- Midwives Have a More Holistic Approach to Healthcare
In general, nurse-midwives tend to have more time to answer all your questions. They can help you learn about the physical and emotional changes you experience as you prepare for your expanding family or with your general care.For those who are expecting, births overseen by CNMs usually have less intervention – such as continuous electronic fetal monitoring, epidurals, and episiotomies – often with better outcomes for women and their babies. Studies have clearly shown that women using CNMs have much lower rates of cesareans.
- Midwives Can Help with Family Planning
A CNM can be a great resource before you have children by assisting with family planning. CNMs also provide contraceptive counseling and services, including prescriptions for oral contraceptive pills, IUD insertions and removals, insertion and removal of hormone-releasing birth control implants. - Certified-Midwives Are Qualified to Care for Women Long-term
This is just like an annual exam with a gynecologist. The midwife does a complete physical exam including a vaginal exam, takes a PAP smear, breast exam and will discuss relevant health topics with you such as family care and nutrition. Many women opt for a midwife because they feel their midwife is someone who is willing to invest personal time and attention in their needs. Certified midwives can also assist women as they enter menopause and face hormonal issues. - Certified Nurse-Midwives Are RNs, Have A Master’s and/or Doctoral Degree in Nursing, and National Certification and Licensure in the State in Which They Work
This preparation qualifies them to perform examinations, order lab tests, prescribe medications, etc. So, pregnant or not, they are a great resource for overall family care. If a pregnancy occurs, you can rest assured they are trained to assist you in having the most healthy and happy pregnancy and birth that is possible. And, CNMs have relationships with physicians in case there is a high-risk situation. - They Offer Access to Additional Holistic Resources
Another great reason to become connected with a nurse-midwife is the opportunity to tap into their network. They are often entrenched in their communities, and can offer great recommendations on other natural, holistic providers. They regularly work with massage therapists, acupuncturists, doulas and yoga therapists. Don’t hesitate to ask for referrals whether you are expecting or not.
Midwife Appointments at DelVal OB/GYN
Giving birth is one of life’s most wonderful and amazing events. The entire team at Delaware Valley OB/GYN considers it a privilege to be entrusted with assisting women in having a healthy pregnancy, birth, and newborn. You can schedule an appointment with a midwife just like scheduling an appointment with a physician at our Practice HERE. And, our midwives participate in OB call for deliveries 24/7.
This is an added dimension of choice provided to you for convenience and satisfaction.
Now Offering TeleHealth Visits

Your safety during the Coronavirus crisis is our utmost concern. In order to keep you and your loved ones safe, our OBGYN doctors, midwives and fertility specialist are now live offering TeleHealth virtual visits.
Here’s how you can get started:
Telehealth appointments are made by phone. Call us during business hours at 609-896-0777 to schedule your virtual visit.
Your can also click here to send us your request online and will be back to you shortly.
You will receive an appointment confirmation for your Telehealth visit by email and/or text shortly from Otto health after your appointment is scheduled. Please click on the links to make sure your device including the speaker and microphone are working properly.
You will get another email and/or text for your Telehealth just before the appointment. Please complete the intake questions and intake forms so you will be allowed into the visit. Give yourself at least 15 minutes to be sure you are ready.
Click Join Visit and you will be connected with your doctor or midwife shortly for your Telehealth appointment.
A couple of tips to make your virtual visit a success,
- Be sure to confirm your Telehealth appointment, test your device and login in for your appointment well in advance.
- Use the right browser: Iphone (safari), Android phone (chrome), Computer (chrome, safari or firefox). Internet explorer and microsoft edge will not work.
- Make sure your wifi or cellular signal is strong and secure.
Having your baby at Penn Medicine Princeton Medical Center

Our doctors and midwives will deliver your baby at Penn Medicine Princeton Medical Center in Plainsboro, NJ. Read their manual ( or click on the image) to learn more about what to expect when your getting ready to deliver at Princeton.
Our commitment to our patients and community
In these difficult times for all of us, the doctors, midwives and staff at Delaware Valley OBGYN and Infertility Group recommit ourselves to treating all of our patients equally and with the dignity that each individual deserves. It is the policy of Delaware Valley Ob/Gyn not to discriminate with regard to race, religion, national origin, socioeconomic status, age, sexual orientation, or disability
Miranda Peurala, CNM joins our team

In the last few months, most of us here in New Jersey and beyond have been pre-occupied with the coronavirus pandemic. In 2020, we had a new addition to our team and are excited to finally share this news with you.
Miranda Peurala, Certified Nurse Midwife, has joined our excellent team of midwives and obstetrician-gynecologists in our Lawrenceville and Princeton and at Penn Medicine Princeton Health. We are thrilled to have her as part of our integrated team that offers our patients the best of all worlds, the personal touch and low c-section rate of a nurse midwife, the easy access to an obstetrician should you need a section or have medical complications during pregnancy, the availability of pain control such as a epidural and the safety of delivering in a hospital with a CHOP (Children’s Hospital of Philadelphia) nursery and the ability to handle emergencies should they arise.
A little bit about Miranda’s training:
- Associate Degree in Nursing: Rowan College at Burlington County
- Bachelor of Science in Nursing: Thomas Edison Statue University
- Master of Science in Nursing – Midwifery: Frontier University
- Certified Lactation Consultant-International Board of Lactation Consultant Examiners (IBLCE)
Please join us in welcoming Miranda to Delaware Valley OBGYN and Infertility Group.
Now scheduling annual exams again

Is it time to schedule my annual gynecologic exam?
If you had your annual check up scheduled with us in the last few months, your visit was almost certainly cancelled, and if you called us to set up an exam, we were unable to schedule the appointment. It was important at the time to limit non-urgent appointments to flatten the curve and to keep our patients and staff safe. However, there is more to good health than just avoiding the coronavirus. Your reproductive and general health is still important, and the annual visit to the gynecologist is part of this. Reproductive healthcare is actually considered an essential service by the authorities in ours and nearby states. Our local hospitals are also now beginning to schedule elective surgeries again.
What do I need to do if I want schedule an annual exam?
We have trying to reach patients whose appointments have been cancelled due to COVID-19 to reschedule, but given the large number of cancellations, it is taking some time. Feel free to call us at 609-896-0777 or use our online form to request an appointment.
Is it safe to come to the office?
The pandemic is easing up but it is not gone. The number of new cases is dropping, but nobody can tell you that you are completely safe from the virus, even at home. Delaware Valley OBGYN’s Lawrenceville office has remained at least partially open so we could be there to serve our pregnant patients. Because of this, we have the experience to know how to keep the office as safe as possible. Our deep cleaning procedures and social distancing procedures have been in place since the early days of the pandemic.
Should I come in if I am high risk?
No. If you are at high risk for getting a serious coronavirus infection (over 65 or with serious medical problems), you should stay home and avoid leaving your home unless it is absolutely essential. We want you to be safe and would love to see you in a few months when the risks of leaving home go down.